Birth Injuries (Including Cerebral Palsy and Brachial Plexus Injuries)
 A birth injury is any injury to a newborn baby’s bodily organs or systems. It can happen during the pregnancy, during labor and delivery, or shortly after birth. Although some birth injuries are minor and heal without any complications, some birth injuries are very serious and result in permanent disability or even death. Serious birth injuries can include brain damage (cerebral palsy, developmental delays, and learning disabilities), other organ damage (heart, lungs, liver, kidneys, etc.), brachial plexus injuries (injury to the nerves that control arm movement, also known as Erb’s palsy and Klumpke’s palsy), and fractured bones.
A birth injury is any injury to a newborn baby’s bodily organs or systems. It can happen during the pregnancy, during labor and delivery, or shortly after birth. Although some birth injuries are minor and heal without any complications, some birth injuries are very serious and result in permanent disability or even death. Serious birth injuries can include brain damage (cerebral palsy, developmental delays, and learning disabilities), other organ damage (heart, lungs, liver, kidneys, etc.), brachial plexus injuries (injury to the nerves that control arm movement, also known as Erb’s palsy and Klumpke’s palsy), and fractured bones.
How Are Birth Injuries Caused?
Each type of birth injury has its own possible causes:
- Brain injury (including cerebral palsy, developmental delays, and learning disabilities): Brain injury is caused by the death of some of the baby’s brain cells. The common causes of brain cell death include hypoxia (lack of oxygen reaching the baby’s brain), hypoglycemia (abnormally low blood sugar), infection, trauma, prematurity, intrauterine growth restriction (“IUGR”), genetic abnormalities, and environmental insult such as maternal alcohol and drug usage, among other causes.
- Brachial plexus injuries (Erb’s palsy or Klumpke’s palsy): These injuries are caused by damage to the baby’s brachial plexus. The brachial plexus is a bundle of nerve fibers between the neck and shoulder that enervate the arm. These injuries result from mechanical forces (trauma) during labor and delivery that tear the nerve fibers and can result in permanent partial or full loss of use of the affected arm. Depending on what part of the brachial plexus is injured, this is called Erb’s palsy or Klumpke’s palsy.
- Bone fractures: These injuries include fractures to the baby’s skull plates and fractured clavicles (a bone in the shoulder). These injuries result from mechanical forces (trauma) during delivery.
- Injury to other bodily organs (heart, lungs, liver, kidneys, etc.): These injuries usually are caused by hypoxia (lack of oxygen reaching the baby’s tissues), although they also be caused by infection, trauma, and other causes.
Although birth injuries can occur without medical error, medical errors can and do cause birth injuries. Click here for examples of how medical errors can cause birth injuries. If you would like a free evaluation of whether a medical error may have caused your child’s birth injury, contact us or complete the form on the left.
What is Cerebral Palsy?
One of the more serious of the various birth injuries is cerebral palsy. Cerebral palsy (“CP”) is the term used for a group of neurological disorders that appear in infancy or early childhood and that cause permanent problems with movement and posture. It is caused by abnormal development of, or damage to, the motor control centers of the brain, usually the motor areas of the brain’s outer layer (called the cerebral cortex). The term cerebral refers to the brain, and palsy refers to the loss or impairment of motor function. The abnormalities of muscle control that define CP are often accompanied by other neurological and physical abnormalities.
 In some cases, the cerebral motor cortex doesn’t develop normally during fetal growth. In other cases, CP is the result of injury to the brain occurring before, during, or after birth (the “prenatal,” “perinatal,” and “postnatal” periods). Although oftentimes there is nothing that could have been done to have prevented the CP, there are times when CP is caused by medical errors.
In some cases, the cerebral motor cortex doesn’t develop normally during fetal growth. In other cases, CP is the result of injury to the brain occurring before, during, or after birth (the “prenatal,” “perinatal,” and “postnatal” periods). Although oftentimes there is nothing that could have been done to have prevented the CP, there are times when CP is caused by medical errors.
The symptoms of CP differ in type and severity from one person to the next, depending on what part of the brain was injured and how severe the injury is. The symptoms in any particular individual may even change over time. All people with cerebral palsy have problems with movement and posture. Children and adults with the severest cases of CP are unable to walk or even roll over on their own. People with CP can also have seizures, abnormal physical sensations or perceptions, and some level of intellectual disability, as well as other medical disorders such as impaired vision, impaired hearing, and language and speech problems.
There is no cure for cerebral palsy, but supportive treatments, medications, and surgery can help many individuals improve their motor skills and ability to communicate with the world.
What Are the Early Signs of CP?
The signs of cerebral palsy usually appear in the early months of life, although a specific diagnosis may be delayed until age two years or later. Infants with CP frequently have developmental delay, in which they are slow to reach developmental milestones such as learning to roll over, sit, crawl, or walk. Some infants with CP have abnormal muscle tone. Decreased muscle tone (hypotonia) can make them appear relaxed, even floppy. Increased muscle tone (hypertonia) can make them seem stiff or rigid. In some cases, an early period of hypotonia will progress to hypertonia after the first 2 to 3 months of life. Children with CP may also have unusual posture or favor one side of the body when they reach, crawl, or move. It is important to note that some children without CP also might have some of these signs.
Some early warning signs of CP:
In a Baby Younger Than 6 Months of Age:
- His head lags when you pick him up while he’s lying on his back
- He feels stiff
- He feels floppy
- When you pick him up, his legs get stiff and they cross or scissor
In a Baby Older Than 6 Months of Age:
- She doesn’t roll over in either direction
- She cannot bring her hands together
- She has difficulty bringing her hands to her mouth
- She reaches out with only one hand while keeping the other fisted
In a Baby Older Than 10 Months of Age:
- He crawls in a lopsided manner, pushing off with one hand and leg while dragging the opposite hand and leg
- He cannot stand even when holding onto support
If you suspect that your child may have CP, contact us or complete the form on the left. We will evaluate (for free) whether any CP that your child may have may have been caused by medical error.
The National Institute of Neurological Disorders and Stroke (“NINDS”) website (part of the U.S. National Institutes of Health) contains an excellent, in-depth discussion of cerebral palsy (last known to be available at <http://www.ninds.nih.gov/disorders/cerebral_palsy/detail_cerebral_palsy.htm>). Likewise, the U.S. Centers for Disease Control and Prevention (“CDC”) also has some excellent, in-depth materials on CP (last known to be available at <http://www.cdc.gov/ncbddd/cp/facts.html>). We refer the reader to these websites for further reading.
What Are the Early Signs of a Brachial Plexus Injury (Erb’s palsy or Klumpke’s palsy)?
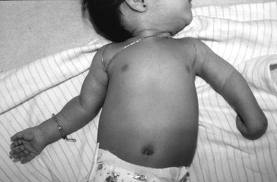 With Erb’s palsy, the early signs and symptoms include:
With Erb’s palsy, the early signs and symptoms include:
- Inability of the baby to move an arm or shoulder, although he can move the fingers
- Affected forearm is extended (straight) and pronated (rotated so that palm faces backwards – see picture to right)
- Reflexes in the affected arm are weak or absent
- There is loss of feeling in the affected arm
With Klumpke’s palsy (which is more rare than Erb’s palsy), the baby will show a “claw hand,” which is the result of paralysis of the intrinsic hand muscle, as well as sensory loss along the ulnar side of the hand and forearm.
Treatment for brachial plexus injuries includes physical therapy and, in some cases, surgery.
For a free case evaluation to see whether your child’s brachial plexus injury may have been caused by medical errors, contact us or complete the form on the left.
Examples of Medical Errors That Can Cause Cerebral Palsy and Other Birth Injuries
 Errors in medical care that cause birth injuries can be grouped by whether they occur in the prenatal period (that is, during the pregnancy), the perinatal period (that is, during labor and delivery), or the postnatal period (that is, shortly after birth, a.k.a. neonatal period).
Errors in medical care that cause birth injuries can be grouped by whether they occur in the prenatal period (that is, during the pregnancy), the perinatal period (that is, during labor and delivery), or the postnatal period (that is, shortly after birth, a.k.a. neonatal period).
- Prenatal Errors – for example:
- Gestational Diabetes — failing to diagnose and address gestational diabetes (a type of diabetes that develops only during pregnancy) and failing to plan for its possible consequences. If early diagnosis and treatment of gestational diabetes is not done, it can lead to a very large (“macrosomic”) baby, which in turn increases the risk of certain serious complications (including brain injury and death). This is because macrosomic babies are at higher risk of being too large to safely fit through the mother’s birth canal (which, if vaginal birth is attempted, can cause skull fractures, brain damage [including cerebral palsy], and brachial plexus injuries to the infant, among other things). Macrosomic babies are also at higher risk of being born prematurely, of experiencing respiratory distress syndrome, of being born hypoglycemic (abnormally low blood sugar, which can cause seizures and brain damage in the newborn), and of having jaundice (abnormally high levels of bilirubin, which can be dangerous if not carefully monitored and treated). Mothers who develop gestational diabetes are at higher risk of developing preeclampsia and eclampsia, two dangerous conditions of pregnancy that cause high blood pressure and other symptoms that can threaten the lives of both mother and baby.
- Placental Problems — failing to diagnose and plan for the consequences of placental abnormalities such as placenta previa (where the placenta grows in the lowest part of the womb and covers all or part of the opening of the cervix) or placental abruption (where the placenta partially or sometimes totally separates from the uterus of the mother). Both placenta previa and partial placental abruption put the baby at higher risk of certain serious complications, including brain injury and death, and complete placental abruption often is fatal to the baby, unless it occurs in a hospital setting where delivery can be immediately effected. The mother likewise is put at risk of serious complications or death by these conditions.
- IUGR — failing to identify and treat “IUGR” (intrauterine growth restriction, a condition where the fetus is smaller than it should be). IUGR puts the baby at risk of various serious health problems, including brain injury and death. There are many potential causes IUGR, but most often it is caused by either poor maternal nutrition or lack of adequate oxygen supply to the baby (which can occur for various reasons). IUGR babies have decreased stores of glycogen and lipids and are less able to withstand the stress of labor and delivery. At birth, they are more likely to have low blood sugar, lower resistance to infection, and trouble maintaining their body temperature. They’re also more prone to high levels of bilirubin (jaundice) and to meconium aspiration (where the baby inhales its own stool in the womb or during delivery). Cerebral palsy has been linked to IUGR.
- Amniotic Fluid Problems — failing to detect and properly treat oligohydramnios (a deficiency of amniotic fluid) and polyhydramnios (an excess of amniotic fluid), both of which can put the baby at higher risk of certain serious complications, including brain injury and death. Oligohydramnios is associated with uteroplacental insufficiency, fetal growth restriction, premature rupture of membranes (PROM), preterm premature rupture of membranes (PPROM), preterm birth, meconium aspiration, umbilical cord compression, preeclampsia, placental abruption, and pulmonary hypoplasia (incomplete development of the baby’s lungs), all of which in turn can cause or contribute to cerebral palsy and in some cases the death of the baby. Polyhydramnios increases the risk for premature rupture of membranes (PROM) and preterm premature rupture of membranes (PPROM), IUGR, umbilical cord prolapse, placental abruption, preeclampsia, and premature birth, all of which likewise can cause or contribute to cerebral palsy.
- Cephalopelvic Disproportion — failing during the late pregnancy period to identify and plan for cephalopelvic disproportion (“CPD”), a condition where the baby’s head or body is too large to safely fit through the mother’s birth canal. This can cause, among other things, brain injury and injury to the baby’s brachial plexus (a bundle of nerves between the neck and shoulder on each side that enervate the arms).
- Preclampsia and Eclampsia — failing to diagnose and properly treat preeclampsia and eclampsia, two dangerous conditions of pregnancy that cause high blood pressure in the mother and other symptoms that can threaten the lives of both mother and baby.
- Post-term Pregnancy — failing to deliver a baby before it becomes post-term. Post-term means that the pregnancy has gone on for more than 42 weeks, which is sufficiently longer than the average such that the baby becomes at higher risk of certain potentially serious problems, including brain injury and death.
- Genetic Defects — failing to identify genetic defects when performing pre-birth screening on the fetus, leading to the birth of a baby with severe birth defects. Washington State recognizes a cause of action for “wrongful birth.”
- Ectopic Pregnancy — failing to identify ectopic pregnancies, which can lead to the mother’s death.
- Diseases and Infections — failing to diagnose a maternal disease or infection that could put the baby at higher risk of certain serious complications, including brain injury and death.
- Labor and Delivery Errors – for example:

- Fetal Distress — failing to diagnose and treat fetal distress, which can lead to brain damage or the death of the baby. During labor and delivery, the baby’s heart rate and the mother’s contractions are checked, usually by using an Electronic Fetal Monitor (“EFM”). These machines produce a strip (fetal monitor strip) that gives clues to the health of the baby during labor and delivery and can show when the baby is undergoing fetal distress (a compromised condition suggesting fetal hypoxia, or insufficient oxygen levels in the fetus). Doctors and nurses at times misinterpret the strip and miss signs of fetal distress, which if appreciated should lead to actions (including, potentially, Caesarian section) that can prevent or lessen brain injury to the baby. Even when doctors and nurses appreciate fetal distress, doctors at times wait too long before performing a Caesarian section.
- Problems with the Progress of Labor — failing to diagnose and appropriately treat inadequate progression of labor (“dystocia of labor”) or other unsafe progression of labor (including excessive molding of the baby’s skull). This can result from a number of factors, including cephalopelvic disproportion (“CPD”), where the baby’s head or body is too large in relation to the mother’s pelvis to safely fit through the pelvis. In cases of cephalopelvic disproportion, the doctor or nurses may allow a trial of labor to go on for too long while augmenting labor with oxytocin or another uterine stimulant. As labor progresses in cases of CPD, the baby’s head is subjected to the trauma of the mother repeatedly attempting to push the head through an opening that is not large enough for it. This can cause or contribute to hypoxia and brain bleeding which in turn can cause brain damage, as well as death. It can also lead to shoulder dystocia, where the baby’s head is born but his/her shoulder gets hung up on the mother’s pubic symphysis. This can cause the baby to have permanent partial or full loss of use of the affected arm.
- Shoulder Dystocia — failing to identify mothers and infants at high risk of shoulder dystocia (where the infant’s head is delivered but one of his/her shoulders gets hung up on the mother’s pubic symphysis, preventing delivery of the rest of the infant), and failing to properly treat shoulder dystocia once it occurs. Improper obstetrical technique during this critical time can result in fetal hypoxia (not enough oxygen to the baby’s brain), potentially resulting in brain damage or death, and can result in damage to the infant’s brachial plexus nerves (a network of nerves on each side running from the neck down through the armpits and into the arms), potentially causing permanent partial or total loss of function of the baby’s upper arm and/or lower arm and hand. This is known as Erb’s palsy or Klumpke’s palsy, depending on the part of the brachial plexus injured.
- Umbilical Cord Problems — failing to appreciate and timely treat problems with the umbilical cord, such as overly tight nuchal cord (cord wrapped around baby’s neck); prolapsed cord (cord below baby’s presenting part), or cord otherwise twisted, knotted, or inadequate. These can lead to compression of the umbilical cord and corresponding decrease in the oxygen reaching the baby’s brain, resulting in brain damage or death.
- Fetal Positioning Problems — failing to recognize and plan for a dangerous presentation of the fetus (for example, breech presentation or shoulder presentation), which can result in brain damage or the death of the baby.
- Technique Problems — improper technique in the use of vacuum extraction or forceps, causing traumatic injury to the baby’s brain and other nerves.
- Postnatal Errors – for example:
- Meconium Aspiration Syndrome — failing to properly treat meconium aspiration syndrome (“MAS”). Meconium is the thick, green stool of the baby while in the uterus. It is normally stored in the baby’s intestines until after birth. However, sometimes meconium is expelled by the baby into the amniotic fluid before birth (that is, the baby passes stool). This usually happens when the baby is under stress. Once the meconium is in the amniotic fluid, the baby can aspirate it (breathe it in) with the amniotic fluid. This can happen either before, during, or immediately after birth. (The baby can “breathe” meconium in while in the womb. This is because babies can mimic breathing motions while still in the womb, even though they obviously do not get any oxygen this way and their oxygen comes from the mother through the umbilical cord and not by “breathing” amniotic fluid.) If the baby aspirates meconium, it can cause airway constriction and blockage after birth. The baby will need to be suctioned to remove the meconium insofar as possible, and the baby may need resuscitation, may need to be placed on a ventilator, and may need various other forms of therapy. Medical errors during the timeframe can cause or exacerbate hypoxia, with resulting brain damage to the infant.
- Hypoglycemia — failing to detect and treat hypoglycemia (abnormally low blood sugar) in the newborn, leading to seizures and potentially brain injury and death. Babies who are at high risk and need screening for hypoglycemia in the first hour of life include newborns who are large for gestational age (weight greater than 90% of other babies after correcting for neonatal sex and ethnicity) or small for gestational age (below 10th percentile) or babies with intrauterine growth restriction (“IUGR”); babies born to insulin-dependent mothers or mothers with gestational diabetes; babies born at a gestational age of less than 37 weeks; babies suspected of sepsis or born to a mother suspected of having chorioamnionitis; and babies showing symptoms suggestive of hypoglycemia, including jitteriness, tachypnea (fast breath rate), hypotonia (poor muscle tone), poor feeding, apnea (temporary pauses in breathing), temperature instability, seizures, and lethargy.
- Resuscitation — failure to properly resuscitate the newborn who has undergone a stressful labor and delivery process.
- High Bilirubin Levels — failing to detect and appropriately treat hyperbilirubinemia (high bilirubin levels, a.k.a. jaundice), which can lead to kernicterus (a type of brain damage) and a certain type of cerebral palsy (choreoathetosis, which is abnormal, uncontrollable writhing movements of the arms and/or legs), as well as oculomotor impairment (problems with eye movement), impaired digestive function, and partial deafness.
- Infection — failing to detect and treat infection (such as bacterial meningitis or other bacterial or viral infection), causing brain and other organ damage.
If you would like a free evaluation of whether a medical error may have caused your child’s birth injury, contact us or complete the confidential form on the left.
We handle cases throughout all of Washington.